Splenic injuries are a significant concern in trauma care, often resulting from blunt or penetrating abdominal trauma. The spleen, a vital organ located in the upper left quadrant of the abdomen, plays a crucial role in the body's immune system and blood filtration. Understanding the Classification of Splenic Injury is essential for healthcare professionals to determine the appropriate management and treatment strategies. This blog post delves into the various classifications of splenic injuries, their diagnostic methods, and the management approaches tailored to each classification.
Understanding Splenic Injuries
Splenic injuries can range from minor lacerations to severe ruptures, each requiring different levels of medical intervention. The spleen’s location and function make it particularly vulnerable to trauma, especially in high-impact accidents or violent incidents. The classification of splenic injuries helps in assessing the severity and guiding the treatment plan.
Classification Systems for Splenic Injuries
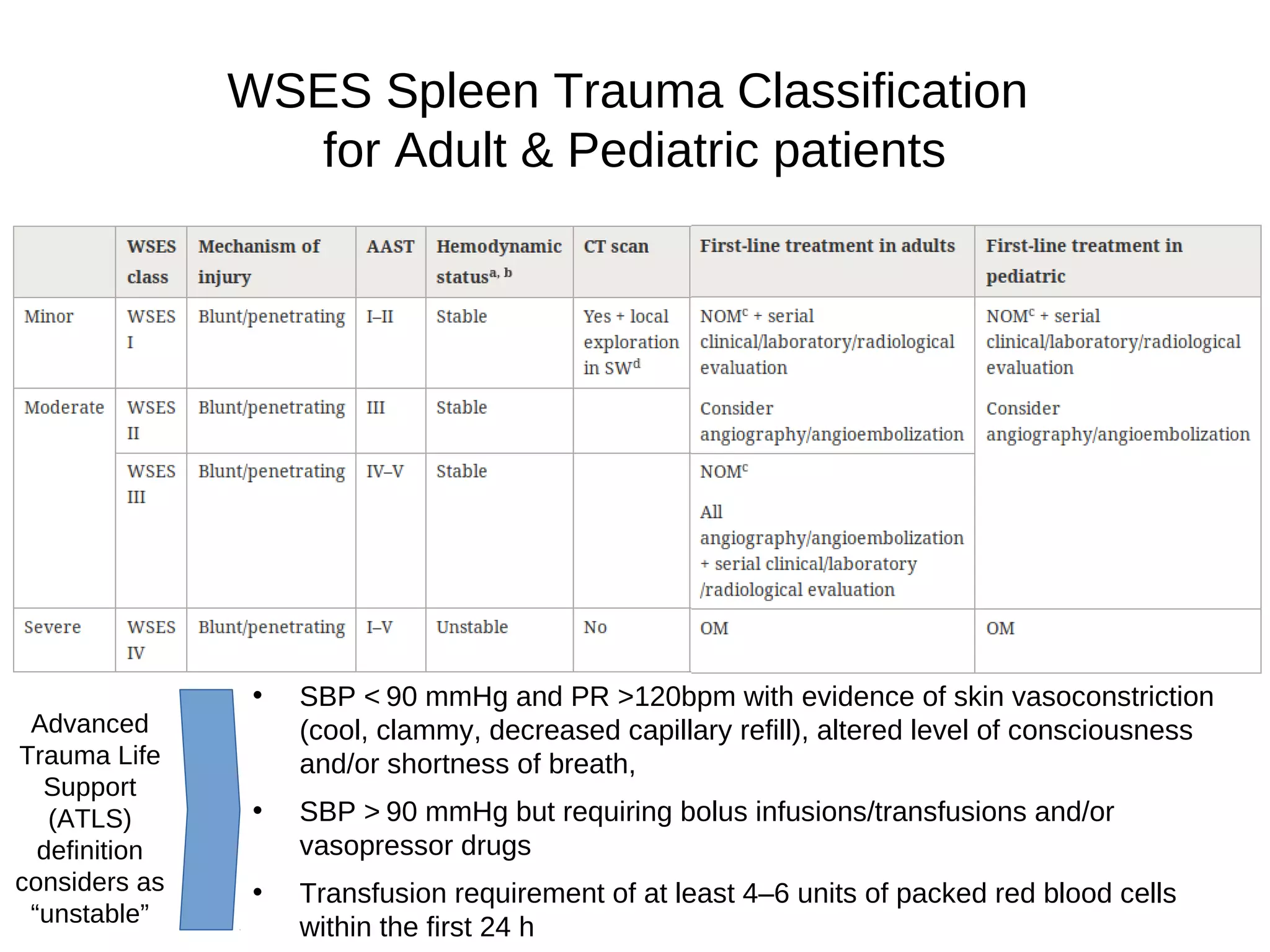
Several classification systems are used to categorize splenic injuries, with the most widely accepted being the American Association for the Surgery of Trauma (AAST) Organ Injury Scale. This scale provides a standardized method for grading the severity of splenic injuries, which is crucial for consistent communication among healthcare providers.
The AAST Organ Injury Scale
The AAST Organ Injury Scale for splenic injuries is divided into six grades, each describing the extent of the injury:
| Grade | Description |
|---|---|
| Grade I | Subcapsular hematoma <10% surface area; capsular tear <1 cm parenchymal depth |
| Grade II | Subcapsular hematoma 10-50% surface area; capsular tear 1-3 cm parenchymal depth; intraparenchymal hematoma <5 cm diameter |
| Grade III | Subcapsular hematoma >50% surface area or expanding; ruptured subcapsular or parenchymal hematoma; intraparenchymal hematoma >5 cm or expanding |
| Grade IV | Laceration involving segmental or hilar vessels producing major devascularization (>25% of spleen) |
| Grade V | Shattered or completely destroyed spleen |
| Grade VI | Hilar vascular injury which devascularizes spleen |
This classification helps in determining the appropriate management strategy, whether it be non-operative management, angiographic embolization, or surgical intervention.
Diagnostic Methods for Splenic Injuries
Accurate diagnosis of splenic injuries is critical for effective management. The primary diagnostic tools include:
- Computed Tomography (CT) Scan: This is the gold standard for diagnosing splenic injuries. CT scans provide detailed images of the spleen and surrounding structures, allowing for precise classification of the injury.
- Ultrasound: While less detailed than CT scans, ultrasound can be useful in initial assessments, especially in unstable patients where a quick evaluation is necessary.
- Diagnostic Peritoneal Lavage (DPL): This invasive procedure involves inserting a catheter into the peritoneal cavity to detect the presence of blood, which may indicate a splenic injury.
Each of these methods has its advantages and limitations, and the choice of diagnostic tool often depends on the patient's stability and the availability of resources.
Management of Splenic Injuries
The management of splenic injuries varies based on the severity of the injury, as classified by the AAST scale. The primary goals are to control bleeding, preserve splenic function, and minimize complications.
Non-Operative Management
Non-operative management is often the preferred approach for lower-grade splenic injuries (Grades I-III). This approach involves close monitoring, bed rest, and serial hematocrit checks. Patients are typically admitted to the hospital for observation, and if they remain stable, they can be discharged with instructions for gradual return to normal activities.
📝 Note: Non-operative management requires a multidisciplinary approach involving trauma surgeons, radiologists, and intensivists to ensure optimal outcomes.
Angiographic Embolization
Angiographic embolization is a minimally invasive procedure used to control bleeding in higher-grade splenic injuries (Grades III-V). This technique involves inserting a catheter into the splenic artery and using embolization coils or other agents to block the bleeding vessel. Embolization can be a lifesaving intervention, especially in patients who are not candidates for surgery.
📝 Note: Embolization is not without risks, including the potential for splenic infarction and abscess formation, so careful patient selection is crucial.
Surgical Intervention
Surgical intervention is necessary for severe splenic injuries (Grades IV-VI) that are not amenable to non-operative management or embolization. Surgical options include splenorrhaphy (repair of the spleen) or splenectomy (removal of the spleen). The choice between these procedures depends on the extent of the injury and the patient’s overall condition.
Splenorrhaphy is preferred when possible to preserve splenic function, as the spleen plays a vital role in immune function, particularly in filtering blood and producing white blood cells. However, in cases of severe injury or hemodynamic instability, splenectomy may be the only viable option.
📝 Note: Patients who undergo splenectomy are at increased risk of overwhelming postsplenectomy infection (OPSI) and should receive appropriate vaccinations and prophylactic antibiotics.
Complications of Splenic Injuries
Splenic injuries can lead to various complications, including:
- Hemorrhage: Continued bleeding from the spleen can lead to hemodynamic instability and shock.
- Infection: Patients with splenic injuries, especially those who undergo splenectomy, are at risk of infections due to the spleen's role in immune function.
- Splenic Abscess: This can occur as a complication of embolization or non-operative management, requiring prompt diagnosis and treatment.
- Pseudocyst Formation: This is a rare complication where a fluid-filled cavity forms within the spleen, which may require surgical intervention.
Early recognition and management of these complications are essential to prevent morbidity and mortality.
Long-Term Considerations
Patients who have experienced splenic injuries, particularly those who have undergone splenectomy, require long-term follow-up and care. This includes:
- Vaccinations: Patients should receive vaccinations against encapsulated bacteria, such as Streptococcus pneumoniae, Haemophilus influenzae type b, and Neisseria meningitidis.
- Prophylactic Antibiotics: Long-term antibiotic prophylaxis may be recommended to reduce the risk of infections.
- Regular Check-ups: Regular follow-up with a healthcare provider to monitor for any signs of infection or other complications.
Education about the risks and symptoms of OPSI is crucial for patients and their families to ensure prompt recognition and treatment of any infections.

Future Directions in Splenic Injury Management
The management of splenic injuries continues to evolve with advancements in diagnostic and therapeutic techniques. Future directions include:
- Advanced Imaging Techniques: The development of more sensitive and specific imaging modalities to improve the accuracy of splenic injury classification.
- Minimally Invasive Procedures: Further refinement of embolization techniques and other minimally invasive procedures to reduce the need for surgical intervention.
- Biomarkers for Injury Severity: Identification of biomarkers that can predict the severity of splenic injuries and guide management decisions.
These advancements aim to improve patient outcomes and reduce the morbidity and mortality associated with splenic injuries.
In summary, the Classification of Splenic Injury is a critical aspect of trauma care, guiding the diagnostic and management strategies for patients with splenic trauma. Understanding the AAST Organ Injury Scale, diagnostic methods, and management approaches is essential for healthcare providers to deliver optimal care. Early recognition, appropriate classification, and timely intervention are key to minimizing complications and improving patient outcomes. Long-term follow-up and education are also crucial for patients who have experienced splenic injuries, particularly those who have undergone splenectomy, to ensure their ongoing health and well-being.
Related Terms:
- aast classification of splenic injury
- splenic laceration grading and management
- grade 5 spleen laceration
- splenic laceration grading scale
- splenic injury grading aast
- splenic injury management guidelines