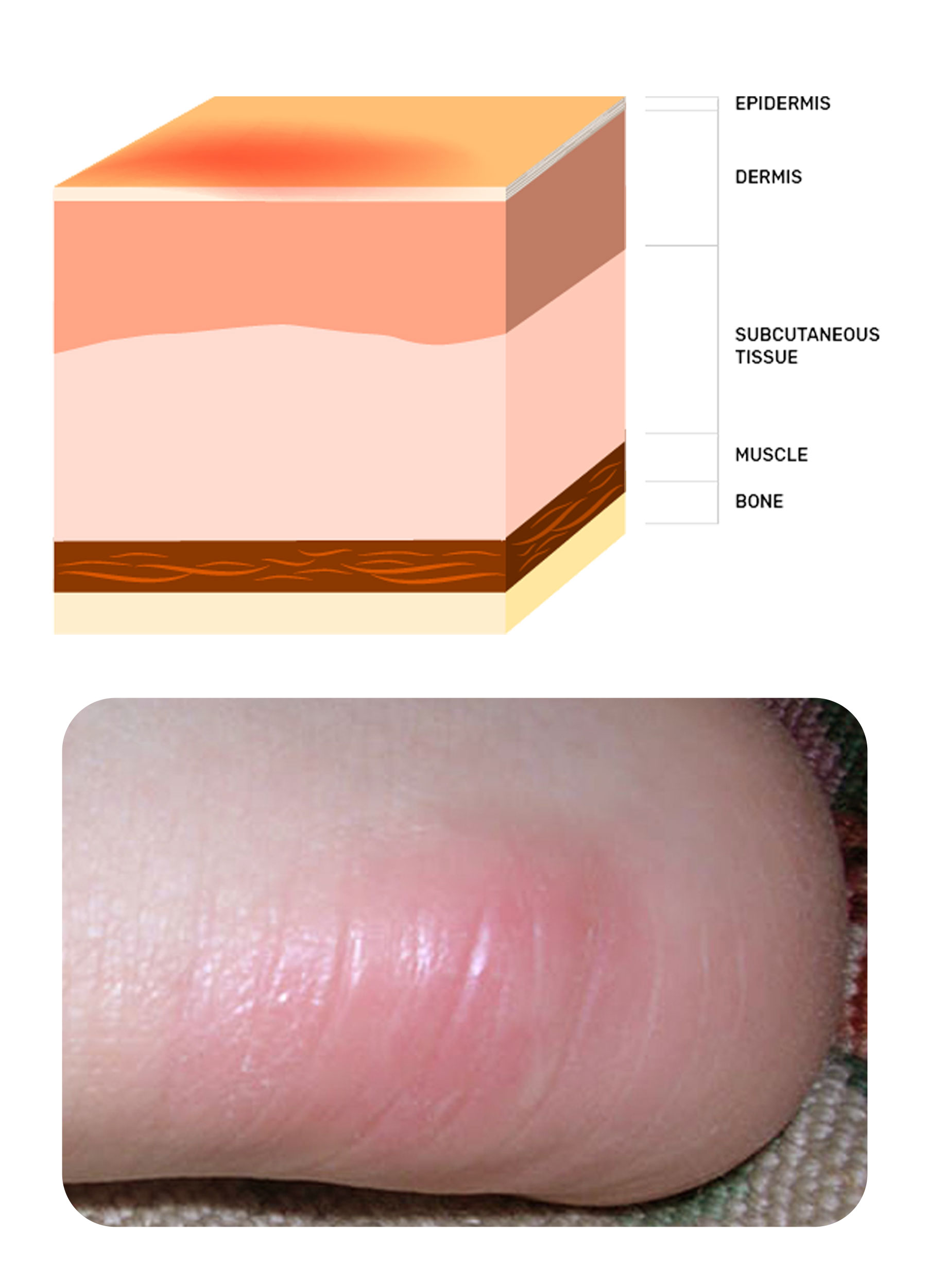
Deep Tissue Pressure Injury (DTPI) is a serious medical condition that affects individuals who are immobile or have limited mobility. This type of injury occurs when prolonged pressure is applied to the skin and underlying tissues, leading to damage and potential tissue death. Understanding the causes, prevention, and treatment of DTPI is crucial for healthcare professionals and caregivers to ensure the well-being of their patients.
Understanding Deep Tissue Pressure Injury
Deep Tissue Pressure Injury refers to damage to the skin and underlying tissues due to prolonged pressure, typically over bony prominences. This condition is often seen in patients who are bedridden, wheelchair-bound, or have limited mobility. The prolonged pressure reduces blood flow to the affected area, leading to tissue ischemia and eventually necrosis if not addressed promptly.
DTPI can occur in various parts of the body, but it is most commonly found over bony areas such as the heels, elbows, hips, and tailbone. The severity of the injury can range from mild redness to deep ulcers that penetrate through the skin and into the muscle and bone.
Risk Factors for Deep Tissue Pressure Injury
Several factors increase the risk of developing a Deep Tissue Pressure Injury. Understanding these risk factors can help in implementing preventive measures. Some of the key risk factors include:
- Immobility: Patients who are bedridden or wheelchair-bound are at a higher risk due to prolonged pressure on specific areas.
- Malnutrition: Poor nutrition can weaken the skin and underlying tissues, making them more susceptible to injury.
- Incontinence: Prolonged exposure to moisture from urine or feces can break down the skin, increasing the risk of DTPI.
- Friction and Shear: Movement that causes friction or shear forces can damage the skin and underlying tissues.
- Medical Conditions: Conditions such as diabetes, vascular disease, and peripheral neuropathy can impair blood flow and sensation, increasing the risk of DTPI.
- Age: Older adults are more prone to DTPI due to thinner skin and reduced tissue elasticity.
Prevention of Deep Tissue Pressure Injury
Preventing Deep Tissue Pressure Injury involves a multi-faceted approach that includes regular skin assessments, proper positioning, and the use of supportive devices. Here are some key strategies for prevention:
Regular Skin Assessments: Conducting regular skin assessments can help identify early signs of DTPI. Look for redness, swelling, warmth, or changes in skin texture. Early detection allows for prompt intervention and prevention of further damage.
Proper Positioning: Regularly changing the patient's position can help reduce prolonged pressure on specific areas. Use pillows, wedges, or other supportive devices to keep the skin off bony prominences. For example, placing a pillow under the heels can prevent pressure on the heels.
Use of Supportive Devices: Specialized mattresses, overlays, and cushions can help distribute pressure more evenly, reducing the risk of DTPI. These devices are designed to minimize pressure points and promote better blood flow.
Maintaining Good Hygiene: Keeping the skin clean and dry is essential for preventing DTPI. Regularly clean the skin and use moisturizers to keep it hydrated. For incontinent patients, use barrier creams to protect the skin from moisture.
Nutritional Support: Ensuring adequate nutrition is crucial for maintaining healthy skin and tissues. A balanced diet rich in proteins, vitamins, and minerals can help strengthen the skin and promote healing.
Managing Medical Conditions: Proper management of underlying medical conditions such as diabetes and vascular disease can help reduce the risk of DTPI. Regular monitoring and treatment can improve blood flow and sensation, making the skin more resistant to injury.
📝 Note: Regularly changing the patient's position is crucial. Aim to change the position every 2 hours to prevent prolonged pressure on any single area.
Treatment of Deep Tissue Pressure Injury
If a Deep Tissue Pressure Injury is detected, prompt and appropriate treatment is essential to prevent further damage and promote healing. The treatment approach depends on the severity of the injury and may include the following steps:
Assessment and Documentation: Thoroughly assess the injury and document its size, depth, and characteristics. This information is crucial for monitoring progress and adjusting the treatment plan as needed.
Wound Care: Clean the wound regularly using sterile saline or other approved solutions. Remove any dead tissue (debridement) to promote healing. Apply appropriate dressings to keep the wound clean and moist, which aids in the healing process.
Pain Management: Manage pain effectively to ensure the patient's comfort and compliance with treatment. Use analgesics as prescribed and consider non-pharmacological methods such as positioning and distraction techniques.
Nutritional Support: Ensure the patient receives adequate nutrition to support wound healing. A diet rich in proteins, vitamins, and minerals can help strengthen the skin and promote tissue repair.
Offloading Pressure: Use supportive devices such as special mattresses, overlays, or cushions to offload pressure from the affected area. This helps reduce further damage and promotes healing.
Regular Monitoring: Monitor the wound regularly for signs of infection or deterioration. Adjust the treatment plan as needed based on the wound's progress.
📝 Note: Always follow the healthcare provider's instructions for wound care and treatment. Proper wound management is crucial for preventing complications and promoting healing.
Complications of Deep Tissue Pressure Injury
If left untreated, Deep Tissue Pressure Injury can lead to several complications, including:
- Infection: Open wounds are susceptible to bacterial infections, which can spread to deeper tissues and even the bloodstream, leading to sepsis.
- Cellulitis: A bacterial infection of the skin and underlying tissues that can cause redness, swelling, and pain.
- Osteomyelitis: An infection of the bone that can occur if the injury penetrates through the skin and into the bone.
- Sepsis: A severe infection that spreads through the bloodstream, affecting multiple organs and potentially leading to organ failure.
- Amputation: In severe cases, the injury may require amputation to prevent the spread of infection and save the patient's life.
Deep Tissue Pressure Injury in Different Patient Populations
Deep Tissue Pressure Injury can affect various patient populations, including:
Elderly Patients: Older adults are at a higher risk due to thinner skin, reduced tissue elasticity, and increased likelihood of immobility. Regular skin assessments and proper positioning are crucial for preventing DTPI in this population.
Patients with Spinal Cord Injuries: Individuals with spinal cord injuries are at a high risk of DTPI due to immobility and reduced sensation. Regular skin checks and the use of supportive devices are essential for prevention.
Patients with Diabetes: Diabetes can impair blood flow and sensation, increasing the risk of DTPI. Proper management of blood sugar levels and regular foot care are crucial for preventing injuries.
Patients with Vascular Disease: Conditions such as peripheral artery disease can reduce blood flow to the extremities, making the skin more susceptible to injury. Regular monitoring and treatment of vascular conditions can help prevent DTPI.
📝 Note: Tailor preventive measures to the specific needs of the patient population. Regular assessments and individualized care plans are essential for effective prevention and management of DTPI.
Deep Tissue Pressure Injury Prevention and Management Protocols
Implementing standardized protocols for the prevention and management of Deep Tissue Pressure Injury can help ensure consistent and effective care. Here are some key components of a comprehensive protocol:
Risk Assessment: Conduct regular risk assessments to identify patients at high risk of DTPI. Use validated tools such as the Braden Scale to assess risk factors and develop individualized prevention plans.
Skin Care: Implement a skin care protocol that includes regular skin assessments, cleaning, and moisturizing. Use barrier creams to protect the skin from moisture and friction.
Positioning and Supportive Devices: Develop a positioning protocol that includes regular changes in position and the use of supportive devices. Ensure that all caregivers are trained in proper positioning techniques.
Nutritional Support: Provide nutritional support to ensure adequate intake of proteins, vitamins, and minerals. Monitor the patient's nutritional status and adjust the diet as needed.
Education and Training: Provide education and training for healthcare professionals and caregivers on the prevention and management of DTPI. Ensure that all staff are aware of the protocol and follow it consistently.
Regular Monitoring and Documentation: Implement a system for regular monitoring and documentation of skin condition and wound progress. Use standardized forms and tools to ensure consistency and accuracy.
📝 Note: Regularly review and update the protocol to ensure it remains effective and up-to-date with the latest evidence-based practices.
Deep Tissue Pressure Injury and Technology
Advancements in technology have led to the development of innovative tools and devices for the prevention and management of Deep Tissue Pressure Injury. Some of these technologies include:
Pressure Mapping Systems: These systems use sensors to map pressure distribution on the skin, identifying areas at risk of DTPI. They can help caregivers adjust positioning and supportive devices to reduce pressure.
Smart Mattresses and Overlays: These devices use advanced materials and technology to distribute pressure evenly and reduce the risk of DTPI. They can also monitor the patient's position and alert caregivers to potential issues.
Wound Imaging and Monitoring: Advanced imaging techniques such as ultrasound and infrared thermography can help monitor wound healing and detect early signs of infection. These tools can provide valuable information for adjusting the treatment plan.
Telemedicine and Remote Monitoring: Telemedicine platforms allow healthcare professionals to monitor patients remotely, providing timely interventions and adjustments to the care plan. Remote monitoring devices can track skin condition and alert caregivers to potential issues.
📝 Note: While technology can be a valuable tool, it should be used in conjunction with regular assessments and individualized care plans. Technology should enhance, not replace, human care.
Deep Tissue Pressure Injury and Patient Education
Educating patients and their caregivers about Deep Tissue Pressure Injury is crucial for prevention and effective management. Here are some key points to include in patient education:
Understanding DTPI: Explain what DTPI is, how it occurs, and the risk factors associated with it. Use simple language and visual aids to ensure understanding.
Prevention Strategies: Teach patients and caregivers about preventive measures such as regular positioning, skin care, and the use of supportive devices. Provide practical tips and demonstrations.
Early Detection: Educate patients and caregivers on the signs of DTPI and the importance of early detection. Encourage regular skin assessments and prompt reporting of any changes.
Wound Care: Provide instructions on proper wound care, including cleaning, dressing, and monitoring. Ensure that patients and caregivers understand the importance of following the treatment plan.
Nutritional Support: Emphasize the role of nutrition in wound healing and provide guidance on maintaining a balanced diet. Offer resources and support for nutritional needs.
📝 Note: Tailor education to the specific needs and abilities of the patient and caregiver. Use a variety of teaching methods and materials to ensure understanding and compliance.
Deep Tissue Pressure Injury and Healthcare Settings
Deep Tissue Pressure Injury can occur in various healthcare settings, including hospitals, long-term care facilities, and home care. Each setting has unique challenges and considerations for prevention and management. Here are some key points for different healthcare settings:
Hospitals: In hospitals, patients may be immobile due to illness or surgery, increasing the risk of DTPI. Regular skin assessments, proper positioning, and the use of supportive devices are crucial. Ensure that all staff are trained in DTPI prevention and management.
Long-Term Care Facilities: In long-term care facilities, residents may have chronic conditions that increase the risk of DTPI. Implement a comprehensive protocol for prevention and management, including regular assessments, skin care, and nutritional support. Provide ongoing education and training for staff.
Home Care: In home care settings, caregivers may not have the same level of training or resources as in healthcare facilities. Provide education and support for caregivers, including regular assessments, skin care, and the use of supportive devices. Encourage open communication and prompt reporting of any changes.
📝 Note: Tailor prevention and management strategies to the specific needs and resources of the healthcare setting. Ensure that all staff and caregivers are trained and supported in DTPI prevention and management.
Deep Tissue Pressure Injury and Research
Ongoing research is essential for advancing the understanding and management of Deep Tissue Pressure Injury. Current research focuses on various aspects of DTPI, including:
Risk Factors and Prevention: Studies are investigating the risk factors associated with DTPI and developing new preventive strategies. Research on pressure mapping systems and smart mattresses is ongoing to improve prevention.
Wound Healing: Research is exploring new treatments and technologies for promoting wound healing. Advanced imaging techniques and telemedicine are being studied to improve monitoring and management.
Patient Outcomes: Studies are evaluating the impact of DTPI on patient outcomes, including quality of life and healthcare costs. Research on the long-term effects of DTPI and the effectiveness of preventive measures is ongoing.
Educational Interventions: Research is focusing on the development and evaluation of educational interventions for patients and caregivers. Studies are investigating the effectiveness of different teaching methods and materials.
📝 Note: Stay informed about the latest research and evidence-based practices in DTPI prevention and management. Incorporate new findings into clinical practice to improve patient outcomes.
Deep Tissue Pressure Injury and Future Directions
As our understanding of Deep Tissue Pressure Injury continues to evolve, so too will the strategies for prevention and management. Future directions in DTPI care may include:
Advanced Technology: The development of new technologies, such as smart sensors and advanced imaging, will enhance our ability to detect and manage DTPI. These tools can provide real-time data and alerts, improving patient outcomes.
Personalized Care: Tailoring prevention and management strategies to the individual needs of patients will become increasingly important. Personalized care plans, based on risk assessments and patient preferences, can improve compliance and effectiveness.
Interdisciplinary Collaboration: Collaboration among healthcare professionals, including nurses, physicians, and therapists, will be crucial for comprehensive DTPI care. Interdisciplinary teams can provide holistic care and support, improving patient outcomes.
Patient and Caregiver Empowerment: Empowering patients and caregivers with knowledge and resources will enhance their ability to prevent and manage DTPI. Education and support can improve compliance and self-management, leading to better outcomes.
📝 Note: Embrace innovation and collaboration in DTPI care. Stay informed about emerging technologies and best practices to provide the highest quality of care.
Deep Tissue Pressure Injury is a serious condition that requires vigilant prevention and prompt treatment. Understanding the causes, risk factors, and preventive measures is essential for healthcare professionals and caregivers. By implementing comprehensive protocols, leveraging technology, and providing education and support, we can significantly reduce the incidence and impact of DTPI. Regular assessments, proper positioning, and nutritional support are key components of effective prevention and management. Collaboration and innovation will continue to drive advancements in DTPI care, improving patient outcomes and quality of life. As we move forward, it is crucial to stay informed about the latest research and best practices, tailoring our approaches to the unique needs of each patient and setting. By doing so, we can ensure that individuals at risk of DTPI receive the best possible care and support, promoting healing and well-being.
Related Terms:
- deep tissue pressure injury management
- deep tissue pressure injury pictures
- deep tissue pressure injury npiap
- evolving deep tissue pressure injury
- deep tissue pressure injury assessment
- deep tissue pressure injury stages