Electrocardiogram (ECG) analysis is a critical tool in cardiology, providing valuable insights into the heart's electrical activity. One of the key features that clinicians look for in an ECG is the ECG Delta Wave. This wave is particularly significant in diagnosing certain cardiac conditions, notably Wolff-Parkinson-White (WPW) syndrome. Understanding the ECG Delta Wave and its implications is essential for accurate diagnosis and effective treatment.
Understanding the ECG Delta Wave
The ECG Delta Wave is a distinctive feature observed in the ECG of patients with WPW syndrome. WPW syndrome is a condition characterized by an accessory pathway that allows electrical impulses to bypass the normal conduction system of the heart. This results in a pre-excitation of the ventricles, leading to the characteristic ECG Delta Wave.
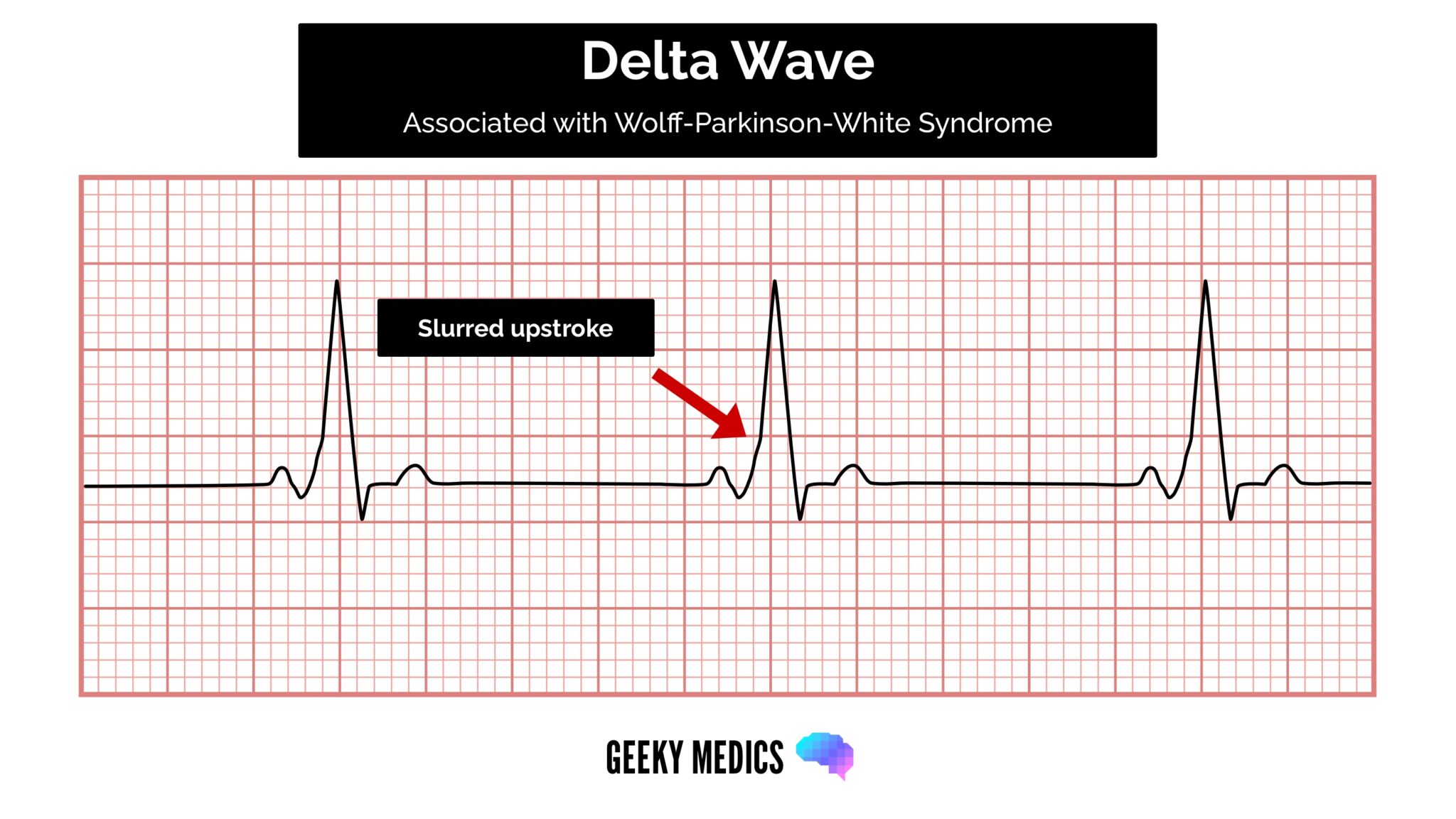
The ECG Delta Wave appears as a slurred upstroke at the beginning of the QRS complex. This slurring is due to the early activation of the ventricles via the accessory pathway, which causes a fusion of the normal QRS complex with the pre-excited QRS complex. The presence of a ECG Delta Wave is a strong indicator of WPW syndrome and requires further investigation to determine the location and properties of the accessory pathway.
Diagnosing WPW Syndrome with the ECG Delta Wave
Diagnosing WPW syndrome involves a thorough analysis of the ECG, with a particular focus on the ECG Delta Wave. The following steps outline the process of diagnosing WPW syndrome using the ECG Delta Wave:
- Identify the Delta Wave: Look for a slurred upstroke at the beginning of the QRS complex. This is the hallmark of the ECG Delta Wave and is indicative of pre-excitation.
- Measure the PR Interval: In WPW syndrome, the PR interval is often shortened due to the early activation of the ventricles. A PR interval of less than 120 milliseconds is a common finding.
- Assess the QRS Complex: The QRS complex in WPW syndrome is typically widened, with a duration of more than 120 milliseconds. This widening is due to the fusion of the normal and pre-excited QRS complexes.
- Determine the Location of the Accessory Pathway: The morphology of the ECG Delta Wave and the QRS complex can provide clues about the location of the accessory pathway. For example, a positive ECG Delta Wave in leads V1 and V2 suggests a left-sided accessory pathway, while a negative ECG Delta Wave in these leads suggests a right-sided pathway.
🔍 Note: The diagnosis of WPW syndrome based on the ECG Delta Wave should be confirmed with additional tests, such as an electrophysiological study, to accurately locate the accessory pathway and plan appropriate treatment.
Clinical Implications of the ECG Delta Wave
The presence of a ECG Delta Wave has significant clinical implications. WPW syndrome can lead to various arrhythmias, including supraventricular tachycardia (SVT), atrial fibrillation, and atrial flutter. These arrhythmias can be life-threatening, especially if they degenerate into ventricular fibrillation. Therefore, prompt and accurate diagnosis of WPW syndrome is crucial for managing these patients effectively.
Treatment options for WPW syndrome include both medical and interventional approaches. Medical management may involve the use of antiarrhythmic drugs to control symptoms and prevent arrhythmias. However, the definitive treatment for WPW syndrome is catheter ablation, a procedure that involves destroying the accessory pathway using radiofrequency energy or cryoablation. This procedure is highly effective in curing WPW syndrome and eliminating the risk of life-threatening arrhythmias.
Interpreting the ECG Delta Wave in Different Clinical Scenarios
The ECG Delta Wave can present differently in various clinical scenarios, and its interpretation requires careful consideration of the patient's clinical context. For example, in patients with atrial fibrillation, the ECG Delta Wave may be obscured by the rapid and irregular ventricular response. In such cases, additional diagnostic tools, such as an electrophysiological study, may be necessary to confirm the presence of WPW syndrome.
In patients with pre-excited atrial fibrillation, the ECG Delta Wave can be particularly challenging to interpret. Pre-excited atrial fibrillation is a life-threatening arrhythmia that occurs when atrial fibrillation is conducted rapidly through the accessory pathway, leading to a very rapid ventricular response. This can degenerate into ventricular fibrillation if not treated promptly. Recognizing the ECG Delta Wave in this context is crucial for initiating appropriate therapy, such as electrical cardioversion or antiarrhythmic drugs.
Advanced Techniques for Analyzing the ECG Delta Wave
Advances in ECG technology have led to the development of sophisticated techniques for analyzing the ECG Delta Wave. These techniques provide more detailed information about the accessory pathway and its properties, aiding in the diagnosis and management of WPW syndrome. Some of these advanced techniques include:
- Signal-Averaged ECG: This technique involves averaging multiple ECG signals to enhance the detection of low-amplitude signals, such as the ECG Delta Wave. It provides a more detailed analysis of the QRS complex and can help in identifying subtle changes in the ECG Delta Wave morphology.
- Vectorcardiography: This technique uses three-dimensional vector analysis to visualize the electrical activity of the heart. It provides a more comprehensive view of the ECG Delta Wave and can help in determining the location and properties of the accessory pathway.
- High-Resolution ECG: This technique involves recording the ECG at a higher sampling rate, allowing for a more detailed analysis of the ECG Delta Wave. It can help in identifying subtle changes in the ECG Delta Wave morphology that may not be apparent on a standard ECG.
🔍 Note: These advanced techniques should be used in conjunction with standard ECG analysis to provide a comprehensive assessment of the ECG Delta Wave and its clinical implications.
Case Studies: Real-World Applications of ECG Delta Wave Analysis
To illustrate the practical application of ECG Delta Wave analysis, consider the following case studies:
Case Study 1: Diagnosis of WPW Syndrome
A 35-year-old patient presented with symptoms of palpitations and dizziness. An ECG was performed, revealing a ECG Delta Wave with a shortened PR interval and widened QRS complex. The ECG Delta Wave was positive in leads V1 and V2, suggesting a left-sided accessory pathway. An electrophysiological study confirmed the presence of WPW syndrome, and the patient underwent successful catheter ablation of the accessory pathway.
Case Study 2: Management of Pre-Excited Atrial Fibrillation
A 40-year-old patient was brought to the emergency department with rapid palpitations and chest pain. An ECG showed a rapid and irregular ventricular response with a ECG Delta Wave, indicative of pre-excited atrial fibrillation. The patient was immediately treated with electrical cardioversion, which restored sinus rhythm. Further evaluation revealed WPW syndrome, and the patient was referred for catheter ablation.
Case Study 3: Challenging Interpretation of the ECG Delta Wave
A 50-year-old patient with a history of hypertension presented with symptoms of fatigue and shortness of breath. An ECG showed a ECG Delta Wave with a shortened PR interval and widened QRS complex. However, the ECG Delta Wave was not clearly visible in all leads, making the diagnosis of WPW syndrome challenging. An electrophysiological study was performed, which confirmed the presence of WPW syndrome and guided the successful ablation of the accessory pathway.
Future Directions in ECG Delta Wave Research
The field of ECG analysis is continually evolving, with ongoing research aimed at improving the detection and interpretation of the ECG Delta Wave. Future directions in this area include:
- Artificial Intelligence and Machine Learning: These technologies have the potential to enhance the accuracy and efficiency of ECG Delta Wave analysis. Machine learning algorithms can be trained to recognize subtle changes in the ECG Delta Wave morphology, aiding in the diagnosis of WPW syndrome and other cardiac conditions.
- Wearable ECG Devices: The development of wearable ECG devices, such as smartwatches and patches, allows for continuous monitoring of cardiac activity. These devices can detect the ECG Delta Wave in real-time, enabling early diagnosis and intervention for WPW syndrome.
- Genetic Studies: Research into the genetic basis of WPW syndrome may provide insights into the mechanisms underlying the ECG Delta Wave. This knowledge can inform the development of targeted therapies and improve patient outcomes.
🔍 Note: Ongoing research and technological advancements hold promise for enhancing the detection and management of the ECG Delta Wave and its associated cardiac conditions.
Conclusion
The ECG Delta Wave is a critical feature in the diagnosis and management of WPW syndrome. Its presence on an ECG provides valuable insights into the heart’s electrical activity and the presence of an accessory pathway. Accurate interpretation of the ECG Delta Wave requires a thorough understanding of its morphology and clinical context. Advanced techniques and ongoing research continue to enhance our ability to detect and manage the ECG Delta Wave, improving patient outcomes and quality of life. By staying informed about the latest developments in ECG analysis, clinicians can provide the best possible care for patients with WPW syndrome and other cardiac conditions.
Related Terms:
- delta wave vs normal ecg
- delta ecg heart health
- delta wave ecg criteria
- delta wave cardiology
- ecg delta effects
- delta sign on ekg