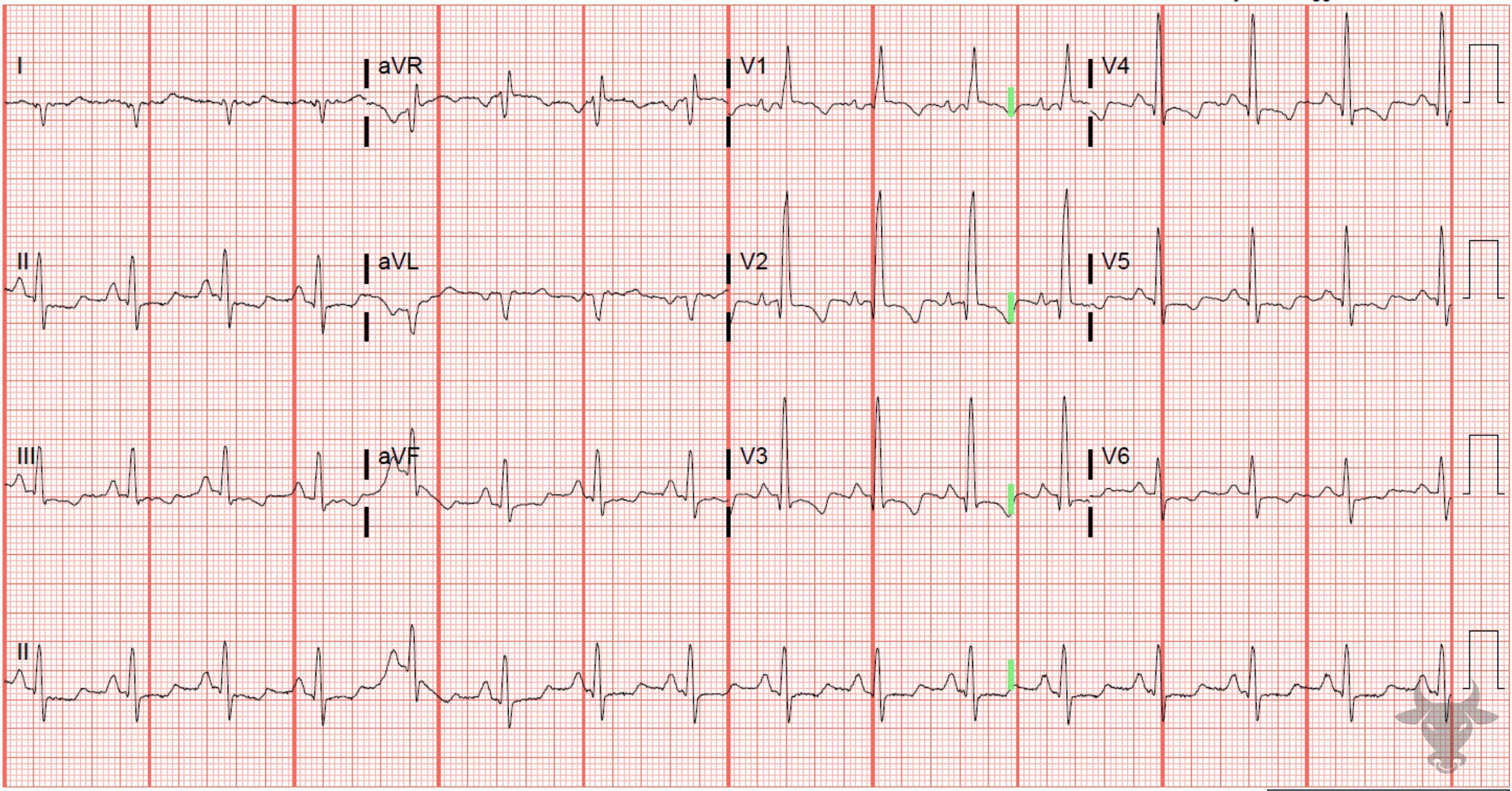
Electrocardiogram (ECG) is a crucial diagnostic tool in cardiology, providing valuable insights into the electrical activity of the heart. Among the various conditions that can be detected through ECG, pulmonary embolism (PE) is one of the most critical. PE is a blockage in one of the pulmonary arteries in the lungs, often caused by a blood clot that travels from elsewhere in the body. Early detection of PE through ECG findings with PE can significantly improve patient outcomes. This blog post delves into the ECG findings associated with PE, their significance, and the diagnostic process.
Understanding Pulmonary Embolism
Pulmonary embolism occurs when a blood clot, typically originating from the deep veins of the legs (deep vein thrombosis or DVT), travels to the lungs and blocks one or more pulmonary arteries. This blockage can lead to reduced blood flow to the lungs, causing symptoms such as shortness of breath, chest pain, and rapid heart rate. In severe cases, PE can be life-threatening.
ECG Findings with PE
ECG is a non-invasive and readily available tool that can provide initial clues about the presence of PE. While ECG findings with PE are not specific and can overlap with other conditions, they are essential in the diagnostic workup. The most common ECG findings in PE include:
- Sinus Tachycardia: An elevated heart rate, often the first sign of PE, indicating the body’s response to the reduced oxygen supply.
- Right Ventricular Strain: This can manifest as T-wave inversions in the right precordial leads (V1-V4), indicating right ventricular overload due to increased pressure in the pulmonary arteries.
- S1Q3T3 Pattern: This classic but rare pattern includes an S wave in lead I, a Q wave in lead III, and an inverted T wave in lead III. It suggests right ventricular strain and is highly suggestive of PE.
- Right Axis Deviation: A shift in the electrical axis of the heart towards the right, indicating right ventricular hypertrophy or strain.
- Atrial Fibrillation: An irregular heart rhythm that can be associated with PE, although it is not specific to this condition.
Diagnostic Workup for PE
While ECG findings with PE can raise suspicion, a definitive diagnosis requires further investigation. The diagnostic workup for PE typically includes:
- D-Dimer Test: A blood test that measures the level of D-dimer, a protein fragment present in the blood after a clot has been broken down. A negative D-dimer test can rule out PE, but a positive result requires further testing.
- Computed Tomography Pulmonary Angiography (CTPA): A CT scan that uses contrast dye to visualize the pulmonary arteries and detect any blockages. CTPA is the gold standard for diagnosing PE.
- Ventilation-Perfusion (V/Q) Scan: A nuclear medicine test that compares the ventilation and perfusion of the lungs. Mismatched areas of ventilation and perfusion can indicate PE.
- Echocardiography: An ultrasound of the heart that can visualize right ventricular strain and other cardiac abnormalities associated with PE.
Interpreting ECG Findings with PE
Interpreting ECG findings with PE requires a systematic approach. The ECG should be reviewed for the presence of sinus tachycardia, right ventricular strain, S1Q3T3 pattern, right axis deviation, and atrial fibrillation. However, it is essential to remember that these findings are not specific to PE and can be seen in other conditions such as acute coronary syndrome, pulmonary hypertension, and chronic obstructive pulmonary disease (COPD).
ECG findings with PE should be correlated with the patient's clinical presentation, risk factors, and results of other diagnostic tests. For example, a patient with a high clinical suspicion of PE, a positive D-dimer test, and ECG findings suggestive of right ventricular strain should undergo further imaging studies such as CTPA or V/Q scan to confirm the diagnosis.
Management of PE
The management of PE depends on the severity of the condition and the patient’s overall health status. Treatment options include:
- Anticoagulation: Medications such as heparin, low-molecular-weight heparin, and warfarin are used to prevent the formation of new clots and the growth of existing clots.
- Thrombolysis: In severe cases, thrombolytic agents such as tissue plasminogen activator (tPA) can be used to dissolve the clot rapidly.
- Inferior Vena Cava (IVC) Filter: A device placed in the inferior vena cava to prevent clots from traveling to the lungs.
- Surgical Embolectomy: A surgical procedure to remove the clot from the pulmonary arteries.
Risk Factors for PE
Understanding the risk factors for PE is crucial for early detection and prevention. Common risk factors include:
- Immobility: Prolonged bed rest, surgery, or travel can increase the risk of blood clots.
- Surgery: Particularly orthopedic surgery, which can increase the risk of DVT and subsequent PE.
- Cancer: Certain types of cancer and cancer treatments can increase the risk of blood clots.
- Pregnancy: The risk of PE is higher during pregnancy and the postpartum period.
- Oral Contraceptives: The use of birth control pills, especially those containing estrogen, can increase the risk of PE.
- Family History: A family history of blood clots or inherited clotting disorders can increase the risk of PE.
Prevention of PE
Preventing PE involves addressing the underlying risk factors and implementing measures to reduce the likelihood of blood clots. Strategies for prevention include:
- Early Mobilization: Encouraging patients to move around as soon as possible after surgery or illness.
- Compression Stockings: Wearing compression stockings to improve blood flow in the legs.
- Anticoagulation: Using anticoagulant medications in high-risk patients to prevent blood clots.
- Hydration: Maintaining adequate hydration to prevent blood from becoming too thick.
📝 Note: While these preventive measures can reduce the risk of PE, it is essential to consult with a healthcare provider to determine the most appropriate strategies based on individual risk factors.
Conclusion
ECG findings with PE play a crucial role in the initial evaluation of patients suspected of having pulmonary embolism. While these findings are not specific to PE, they can provide valuable clues that prompt further diagnostic testing. Early detection and management of PE are essential for improving patient outcomes. Understanding the ECG findings, diagnostic workup, risk factors, and preventive measures for PE can help healthcare providers make informed decisions and provide optimal care for their patients.
Related Terms:
- ekg changes on pe
- signs of pe on ekg
- ekg finding in pe
- ekg findings consistent with pe
- ecg pattern in pe
- ekg changes associated with pe