Wound care is a critical aspect of healthcare, particularly when dealing with complex injuries such as necrotic tissue wounds. These wounds, characterized by the presence of dead or dying tissue, require specialized attention to promote healing and prevent further complications. Understanding the nature of necrotic tissue wounds, their causes, and effective treatment strategies is essential for healthcare professionals and caregivers alike.
Understanding Necrotic Tissue Wounds
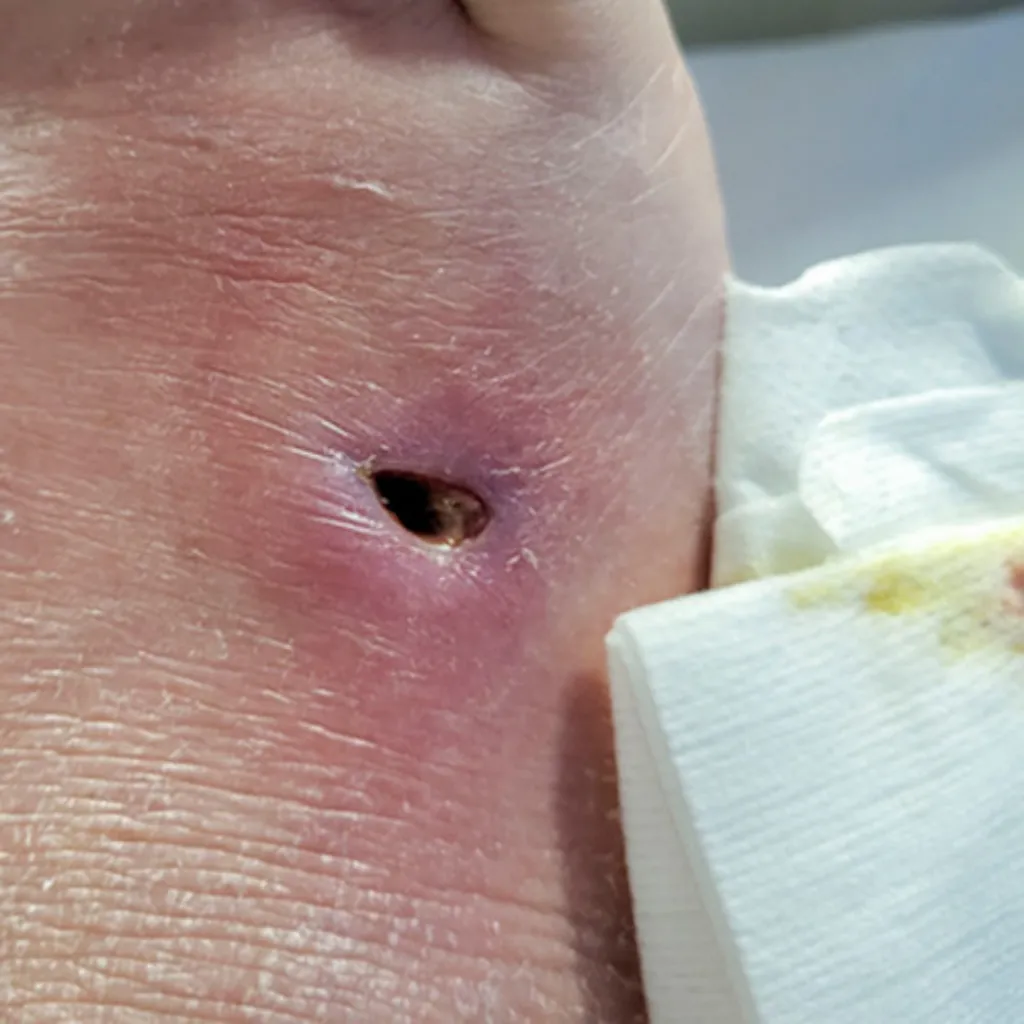
Necrotic tissue wounds occur when tissue dies due to a lack of blood supply, infection, or trauma. This dead tissue can impede the healing process by creating a barrier that prevents new tissue from forming. Necrotic tissue is often yellow, black, or brown in color and may have a foul odor. Common causes of necrotic tissue wounds include:
- Diabetes
- Peripheral artery disease
- Pressure ulcers
- Burns
- Trauma
- Infections
Identifying necrotic tissue is the first step in effective wound management. Healthcare professionals use various assessment tools and techniques to determine the extent and type of necrosis present. This assessment helps in developing a tailored treatment plan.
Assessment and Diagnosis of Necrotic Tissue Wounds
Assessing a necrotic tissue wound involves a thorough examination of the wound bed, surrounding tissue, and the patient's overall health. Key aspects of the assessment include:
- Wound size and depth
- Type of necrosis (dry, wet, or eschar)
- Presence of infection
- Patient's medical history and comorbidities
- Pain levels and patient comfort
Diagnostic tools such as imaging studies, laboratory tests, and microbiological cultures may also be used to gather more information about the wound and the patient's condition. This comprehensive assessment ensures that the treatment plan addresses all aspects of the wound and the patient's health.
Treatment Strategies for Necrotic Tissue Wounds
Effective treatment of necrotic tissue wounds involves several key steps, including debridement, wound cleansing, and the application of appropriate dressings. The goal is to remove the necrotic tissue, promote healing, and prevent infection.
Debridement
Debridement is the process of removing dead, damaged, or infected tissue from a wound. This can be achieved through various methods, including:
- Surgical debridement: Involves the use of surgical instruments to cut away necrotic tissue.
- Mechanical debridement: Uses physical methods such as wet-to-dry dressings or whirlpool therapy to remove dead tissue.
- Enzymatic debridement: Utilizes enzymes to break down and dissolve necrotic tissue.
- Autolytic debridement: Involves the use of moist dressings to promote the body's natural processes to break down dead tissue.
- Biological debridement: Uses maggots to consume necrotic tissue.
Each method has its advantages and is chosen based on the type and extent of necrosis, the patient's overall health, and the healthcare provider's expertise.
📝 Note: Debridement should be performed by trained healthcare professionals to minimize the risk of further tissue damage and infection.
Wound Cleansing
Wound cleansing is a crucial step in managing necrotic tissue wounds. It involves removing debris, bacteria, and exudate from the wound bed. Common cleansing solutions include:
- Normal saline
- Povidone-iodine
- Chlorhexidine
- Hydrogen peroxide
The choice of cleansing solution depends on the wound's condition and the presence of infection. Gentle cleansing techniques, such as irrigation with a syringe or gentle wiping with gauze, are preferred to avoid further tissue damage.
📝 Note: Avoid using harsh chemicals or excessive force during wound cleansing to prevent further tissue trauma.
Dressing Selection
Selecting the appropriate dressing is essential for promoting healing and managing exudate. Common types of dressings for necrotic tissue wounds include:
- Gauze dressings
- Hydrocolloid dressings
- Foam dressings
- Alginate dressings
- Hydrofiber dressings
Each type of dressing has specific indications and benefits. For example, hydrocolloid dressings are useful for managing moderate to heavy exudate, while foam dressings are ideal for absorbing excess fluid and providing cushioning.
📝 Note: Dressing changes should be performed regularly to monitor the wound's progress and prevent infection.
Advanced Wound Care Therapies
In some cases, advanced wound care therapies may be necessary to promote healing in necrotic tissue wounds. These therapies include:
- Negative pressure wound therapy (NPWT): Uses a vacuum device to apply negative pressure to the wound, promoting drainage and tissue growth.
- Hyperbaric oxygen therapy (HBOT): Involves breathing pure oxygen in a pressurized room to enhance tissue oxygenation and healing.
- Growth factors and biologics: Utilizes substances such as platelet-rich plasma (PRP) or recombinant growth factors to stimulate tissue regeneration.
- Skin substitutes and grafts: Involves the use of artificial or natural skin substitutes to cover the wound and promote healing.
These advanced therapies are often used in conjunction with traditional wound care methods to achieve optimal results.
Preventing Complications in Necrotic Tissue Wounds
Preventing complications is a critical aspect of managing necrotic tissue wounds. Common complications include infection, delayed healing, and the development of chronic wounds. Strategies to prevent these complications include:
- Regular wound assessment and monitoring
- Prompt and thorough debridement
- Appropriate wound cleansing and dressing selection
- Management of underlying conditions such as diabetes and peripheral artery disease
- Patient education on wound care and self-management
By implementing these strategies, healthcare providers can minimize the risk of complications and promote better outcomes for patients with necrotic tissue wounds.
Patient Education and Self-Care
Patient education plays a vital role in the management of necrotic tissue wounds. Educating patients about wound care, self-management, and the importance of follow-up care can significantly improve outcomes. Key areas of patient education include:
- Proper wound cleansing techniques
- Dressing application and removal
- Recognizing signs of infection
- Managing pain and discomfort
- Maintaining a healthy lifestyle to support wound healing
Healthcare providers should also encourage patients to seek prompt medical attention if they notice any changes in the wound or experience increased pain or discomfort.
📝 Note: Patient education should be tailored to the individual's needs and understanding to ensure effective self-care.
Case Studies and Clinical Examples
To illustrate the management of necrotic tissue wounds, consider the following case studies:
Case Study 1: Diabetic Foot Ulcer
A 65-year-old patient with a history of diabetes presents with a necrotic tissue wound on the plantar surface of the foot. The wound is approximately 5 cm in diameter, with a foul odor and yellowish discharge. The patient reports severe pain and difficulty walking.
Assessment reveals a deep ulcer with extensive necrosis and signs of infection. The patient is admitted to the hospital for surgical debridement, followed by negative pressure wound therapy and antibiotic treatment. Regular dressing changes and wound cleansing are performed, and the patient is educated on proper foot care and self-management.
Over the course of several weeks, the wound shows significant improvement, with reduced necrosis and increased granulation tissue. The patient is discharged with instructions for continued wound care and follow-up appointments.
Case Study 2: Pressure Ulcer
A 78-year-old patient with a history of spinal cord injury presents with a stage IV pressure ulcer on the sacrum. The wound is approximately 8 cm in diameter, with black eschar and a foul odor. The patient reports minimal pain but has a history of recurrent infections.
Assessment reveals extensive necrosis and signs of infection. The patient undergoes surgical debridement, followed by enzymatic debridement to remove remaining necrotic tissue. The wound is dressed with a hydrocolloid dressing to manage exudate and promote healing. The patient is also started on antibiotic therapy to treat the infection.
Regular wound assessments and dressing changes are performed, and the patient is educated on pressure relief techniques and proper nutrition to support wound healing. Over time, the wound shows significant improvement, with reduced necrosis and increased granulation tissue.
Conclusion
Managing necrotic tissue wounds requires a comprehensive approach that includes thorough assessment, effective debridement, appropriate wound cleansing, and the use of advanced therapies when necessary. By understanding the causes and treatment strategies for necrotic tissue wounds, healthcare providers can promote better outcomes and improve the quality of life for patients. Regular monitoring, patient education, and the prevention of complications are essential components of successful wound management. Through a multidisciplinary approach and tailored treatment plans, healthcare providers can effectively address the challenges posed by necrotic tissue wounds and support the healing process.