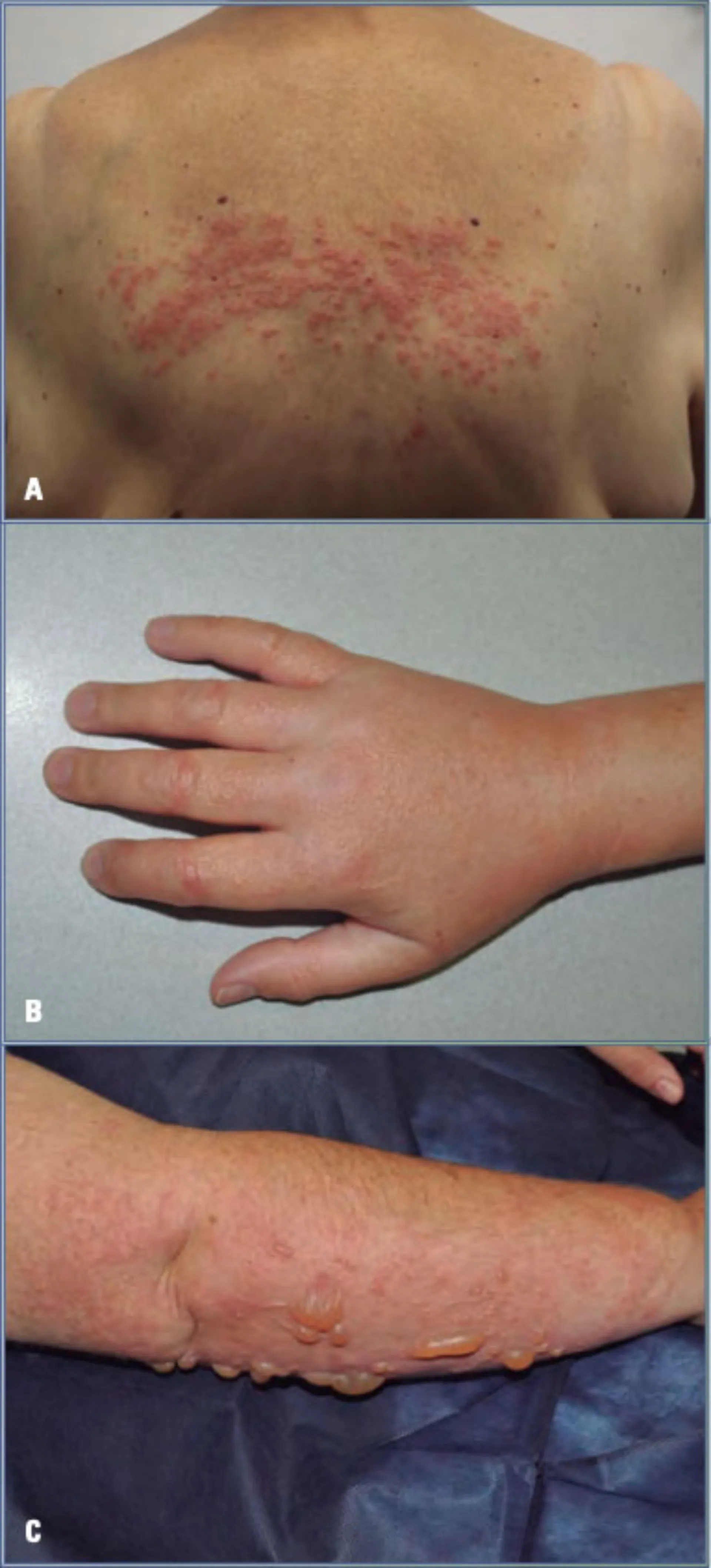
Dermatitis is a common skin condition that affects millions of people worldwide. It is characterized by inflammation of the skin, which can lead to symptoms such as redness, itching, and swelling. Understanding what dermatitis is, its types, causes, and treatment options is crucial for managing this condition effectively. This blog post aims to provide a comprehensive overview of dermatitis, focusing on its various forms, symptoms, and management strategies.
What is Dermatitis?
Dermatitis, often referred to as eczema, is a broad term that encompasses several types of skin inflammation. It is not a single condition but rather a group of conditions that share similar symptoms. The most common types of dermatitis include atopic dermatitis, contact dermatitis, seborrheic dermatitis, and stasis dermatitis. Each type has its unique causes and triggers, but they all result in similar skin reactions.
Types of Dermatitis
Understanding the different types of dermatitis is essential for proper diagnosis and treatment. Here are the most common types:
Atopic Dermatitis
Atopic dermatitis, also known as eczema, is a chronic condition that often begins in childhood. It is characterized by dry, itchy skin and recurrent rashes. The exact cause of atopic dermatitis is unknown, but it is believed to be related to a combination of genetic and environmental factors. People with atopic dermatitis often have a family history of allergies or asthma.
Contact Dermatitis
Contact dermatitis occurs when the skin comes into contact with an irritant or allergen. It can be further divided into two types: irritant contact dermatitis and allergic contact dermatitis. Irritant contact dermatitis is caused by direct irritation of the skin, while allergic contact dermatitis is an immune response to a specific allergen.
Seborrheic Dermatitis
Seborrheic dermatitis is a common condition that affects the scalp, face, and other oily areas of the body. It is characterized by red, scaly patches and dandruff. The exact cause of seborrheic dermatitis is unknown, but it is thought to be related to an overgrowth of a type of yeast that naturally lives on the skin.
Stasis Dermatitis
Stasis dermatitis, also known as venous eczema, occurs when there is poor circulation in the lower legs. It is often associated with varicose veins and other circulatory problems. The condition is characterized by swelling, redness, and itching in the affected area.
Symptoms of Dermatitis
The symptoms of dermatitis can vary depending on the type and severity of the condition. However, some common symptoms include:
- Redness and inflammation of the skin
- Itching and discomfort
- Dry, scaly patches
- Blisters or small bumps
- Crusting or oozing
- Swelling
These symptoms can range from mild to severe and may come and go over time. It is important to seek medical attention if symptoms are persistent or worsening.
Causes and Triggers of Dermatitis
The causes of dermatitis can vary depending on the type. However, some common factors that contribute to the development of dermatitis include:
- Genetic predisposition
- Environmental factors such as allergens, irritants, and pollutants
- Immune system dysfunction
- Hormonal changes
- Stress and anxiety
Identifying and avoiding specific triggers can help manage symptoms and prevent flare-ups. Common triggers include:
- Soaps and detergents
- Certain fabrics, such as wool or synthetic materials
- Allergens, such as pollen, dust mites, or pet dander
- Food allergies
- Extreme temperatures and humidity
Diagnosing Que Es Dermatitis
Diagnosing dermatitis involves a thorough medical history and physical examination. The healthcare provider will ask about symptoms, family history, and any potential triggers. In some cases, additional tests may be necessary to confirm the diagnosis. These tests may include:
- Skin biopsy
- Patch testing
- Blood tests
- Allergy testing
Accurate diagnosis is crucial for developing an effective treatment plan.
Treatment Options for Dermatitis
The treatment of dermatitis depends on the type and severity of the condition. The goal of treatment is to reduce inflammation, relieve symptoms, and prevent future flare-ups. Common treatment options include:
Topical Treatments
Topical treatments are applied directly to the skin and are often the first line of defense against dermatitis. These may include:
- Corticosteroid creams or ointments
- Moisturizers
- Antibiotics
- Antihistamines
Oral Medications
In some cases, oral medications may be prescribed to manage severe or persistent symptoms. These may include:
- Antibiotics
- Antihistamines
- Immunosuppressants
Phototherapy
Phototherapy involves exposing the skin to controlled amounts of natural or artificial light. This treatment can help reduce inflammation and itching. It is often used for severe cases of atopic dermatitis.
Lifestyle Changes
Making lifestyle changes can also help manage dermatitis symptoms. These may include:
- Avoiding known triggers
- Using gentle skincare products
- Wearing loose, breathable clothing
- Maintaining a healthy diet
- Managing stress
Managing Dermatitis at Home
In addition to medical treatments, there are several steps you can take at home to manage dermatitis symptoms. These include:
- Keeping the skin moisturized
- Avoiding hot showers or baths
- Using mild soaps and detergents
- Wearing gloves when handling irritants
- Avoiding scratching the affected area
It is important to follow your healthcare provider’s recommendations and avoid self-medicating without proper guidance.
When to Seek Medical Attention
While mild cases of dermatitis can often be managed at home, it is important to seek medical attention if symptoms are severe or worsening. Signs that you should see a healthcare provider include:
- Persistent or worsening symptoms
- Infection or pus-filled blisters
- Fever or chills
- Difficulty breathing or swallowing
Early intervention can help prevent complications and improve outcomes.
📝 Note: Always consult with a healthcare provider before starting any new treatment or making significant lifestyle changes.
Preventing Dermatitis Flare-Ups
Preventing dermatitis flare-ups involves identifying and avoiding triggers, maintaining good skincare habits, and following your healthcare provider’s recommendations. Some tips for preventing flare-ups include:
- Keeping the skin hydrated
- Using gentle skincare products
- Avoiding known allergens and irritants
- Wearing protective clothing
- Managing stress
Regular check-ups with your healthcare provider can also help monitor your condition and adjust treatment as needed.
Living with Dermatitis
Living with dermatitis can be challenging, but with the right management strategies, it is possible to control symptoms and improve quality of life. It is important to stay informed about your condition, follow your healthcare provider’s recommendations, and seek support when needed. Joining support groups or online communities can provide valuable information and emotional support.
Dermatitis is a common skin condition that affects millions of people worldwide. Understanding the different types, symptoms, and treatment options is crucial for managing this condition effectively. By working closely with your healthcare provider and making necessary lifestyle changes, you can control symptoms and improve your overall well-being.
Related Terms:
- efectos secundarios de dermatitis
- que la dermatitis en piel
- que es dermatitis seborreica
- definicion de dermatitis
- dermatitis en la cara tratamiento
- la dermatitis es contagiosa