Colonoscopy is a crucial medical procedure that plays a vital role in the early detection and prevention of colorectal cancer. This procedure involves the examination of the inner lining of the colon and rectum using a long, flexible tube with a camera and light. Understanding who does colonoscopy and the importance of this procedure can help individuals make informed decisions about their health.
Understanding Colonoscopy
A colonoscopy is typically performed by a healthcare professional known as a gastroenterologist. These specialists are trained to diagnose and treat diseases of the digestive system, including the colon and rectum. The procedure is usually carried out in a hospital or outpatient setting and involves the use of sedation to ensure the patient's comfort.
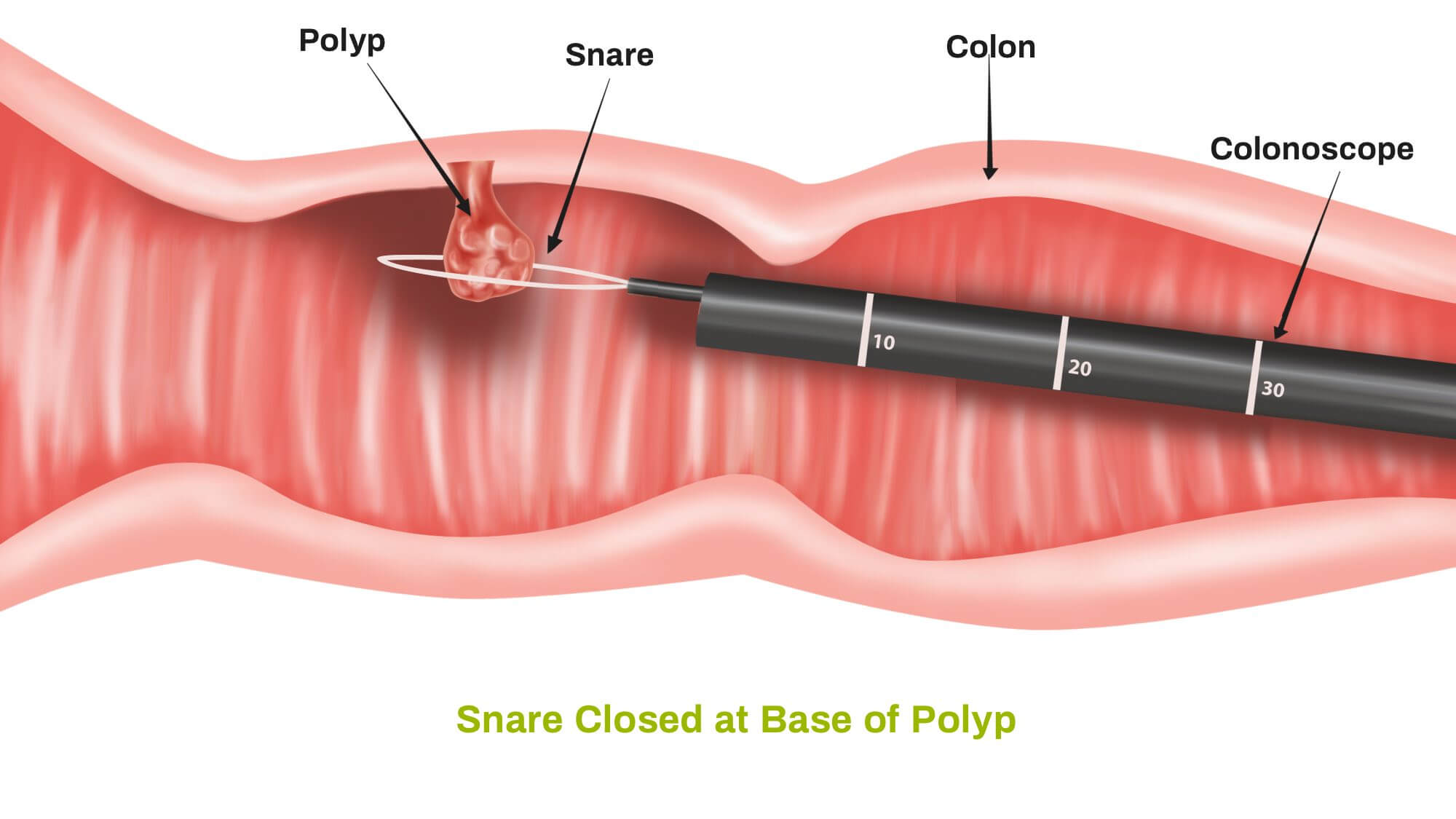
During a colonoscopy, the gastroenterologist inserts a colonoscope—a thin, flexible tube with a camera and light—into the rectum and advances it through the colon. The camera transmits images to a monitor, allowing the doctor to examine the colon's lining for any abnormalities, such as polyps or signs of inflammation. If any polyps are detected, they can be removed during the procedure, and tissue samples can be taken for biopsy.
Who Does Colonoscopy?
The question of who does colonoscopy is often asked by individuals who are scheduled for the procedure or those who are considering it. Colonoscopies are performed by trained medical professionals who specialize in gastrointestinal health. These professionals include:
- Gastroenterologists: These are medical doctors who specialize in the diagnosis and treatment of diseases of the digestive system. They are the primary healthcare providers who perform colonoscopies.
- Colorectal Surgeons: These surgeons specialize in the surgical treatment of diseases of the colon, rectum, and anus. They may also perform colonoscopies, especially in cases where surgical intervention is anticipated.
- General Surgeons: In some cases, general surgeons who have received additional training in colonoscopy may perform the procedure, particularly in rural or underserved areas where gastroenterologists may not be available.
It is essential to note that the training and expertise of the healthcare provider performing the colonoscopy can significantly impact the quality and accuracy of the procedure. Therefore, it is crucial to choose a qualified and experienced professional for this important medical examination.
Preparation for Colonoscopy
Preparing for a colonoscopy is a critical step in ensuring the procedure's success. Proper preparation involves several key steps:
- Dietary Restrictions: Patients are typically advised to follow a clear liquid diet for 24-48 hours before the procedure. This diet includes foods and beverages that are clear and easily digested, such as broth, gelatin, and clear juices.
- Bowel Cleansing: A bowel cleansing regimen is prescribed to empty the colon of stool. This usually involves taking a laxative solution or a series of enemas. The goal is to ensure that the colon is completely clean, allowing the gastroenterologist to have a clear view of the colon's lining.
- Medication Adjustments: Patients may need to adjust or temporarily stop certain medications, such as blood thinners or diabetes medications, before the procedure. It is essential to consult with the healthcare provider about any medications that should be adjusted or stopped.
- Hydration: Staying hydrated is crucial during the preparation phase. Patients should drink plenty of clear liquids to replace fluids lost during bowel cleansing.
Following these preparation steps carefully can help ensure a successful colonoscopy and accurate diagnosis.
📝 Note: Always follow the specific instructions provided by your healthcare provider for colonoscopy preparation, as individual needs may vary.
What to Expect During the Procedure
On the day of the colonoscopy, patients are typically asked to arrive at the medical facility a few hours before the procedure. The following steps outline what to expect during the colonoscopy:
- Check-In and Preparation: Upon arrival, patients will check in and be escorted to a preparation area. They will change into a hospital gown and may be asked to remove any jewelry or other items that could interfere with the procedure.
- Sedation: Before the procedure begins, patients will receive sedation to ensure comfort and relaxation. The type and amount of sedation will depend on the patient's individual needs and the healthcare provider's recommendations.
- The Procedure: The gastroenterologist will insert the colonoscope into the rectum and advance it through the colon. The camera at the tip of the colonoscope transmits images to a monitor, allowing the doctor to examine the colon's lining. If any polyps or abnormalities are detected, they can be removed or biopsied during the procedure.
- Recovery: After the procedure, patients will be taken to a recovery area where they will be monitored until the sedation wears off. Most patients can go home the same day, but it is essential to have someone available to drive them home and stay with them for the rest of the day.
The entire colonoscopy procedure typically takes about 30-60 minutes, although the preparation and recovery time can add several hours to the overall process.
Benefits of Colonoscopy
Colonoscopy offers several significant benefits, making it a crucial tool in the prevention and early detection of colorectal cancer. Some of the key benefits include:
- Early Detection: Colonoscopy allows for the early detection of polyps and other abnormalities in the colon. Early detection can lead to timely intervention and treatment, improving the chances of a positive outcome.
- Prevention: By removing polyps during the procedure, colonoscopy can prevent the development of colorectal cancer. Polyps, if left untreated, can become cancerous over time.
- Diagnosis: Colonoscopy is an effective diagnostic tool for various gastrointestinal conditions, including inflammatory bowel disease, diverticulosis, and other colon-related issues.
- Screening: Regular colonoscopies are recommended for individuals at average risk of colorectal cancer, typically starting at age 45. For those with a family history of colorectal cancer or other risk factors, earlier and more frequent screenings may be advised.
Regular colonoscopies can significantly reduce the risk of colorectal cancer and improve overall health outcomes.
Risks and Complications
While colonoscopy is generally a safe procedure, it is essential to be aware of potential risks and complications. Some of the possible risks include:
- Bleeding: Bleeding can occur if polyps are removed during the procedure. In most cases, bleeding is minor and stops on its own, but in some instances, it may require medical intervention.
- Perforation: There is a small risk of perforation, or a tear in the colon wall, during the procedure. This can lead to infection and may require surgical repair.
- Reactions to Sedation: Some patients may experience adverse reactions to the sedation used during the procedure, such as allergic reactions or breathing difficulties.
- Infection: Although rare, there is a risk of infection associated with colonoscopy. Proper sterilization of equipment and adherence to infection control protocols can minimize this risk.
It is crucial to discuss any concerns about potential risks and complications with the healthcare provider before undergoing a colonoscopy.
📝 Note: Inform your healthcare provider about any allergies, medical conditions, or medications you are taking before the colonoscopy to minimize the risk of complications.
Who Should Get a Colonoscopy?
Colonoscopy is recommended for individuals at average risk of colorectal cancer, typically starting at age 45. However, certain factors may increase the risk of developing colorectal cancer, and in such cases, earlier and more frequent screenings may be advised. Some of the factors that increase the risk of colorectal cancer include:
- Family History: Individuals with a family history of colorectal cancer or polyps are at a higher risk and may need to start screening earlier.
- Personal History: Those who have previously had colorectal cancer or polyps are at a higher risk of developing the disease again.
- Inflammatory Bowel Disease: Conditions such as ulcerative colitis and Crohn's disease increase the risk of colorectal cancer.
- Genetic Syndromes: Certain genetic syndromes, such as familial adenomatous polyposis (FAP) and hereditary nonpolyposis colorectal cancer (HNPCC), significantly increase the risk of colorectal cancer.
- Lifestyle Factors: A diet high in red and processed meats, low in fiber, and high in alcohol consumption, as well as a sedentary lifestyle and smoking, can increase the risk of colorectal cancer.
It is essential to consult with a healthcare provider to determine the appropriate screening schedule based on individual risk factors.
Colonoscopy vs. Other Screening Methods
In addition to colonoscopy, there are other screening methods available for detecting colorectal cancer. Each method has its advantages and limitations. Some of the alternative screening methods include:
| Screening Method | Description | Advantages | Limitations |
|---|---|---|---|
| Fecal Occult Blood Test (FOBT) | A test that detects hidden blood in the stool, which can be a sign of colorectal cancer or polyps. | Non-invasive, easy to perform, and can be done at home. | Less accurate than colonoscopy, may require follow-up colonoscopy if positive. |
| Fecal Immunochemical Test (FIT) | A test that detects human hemoglobin in the stool, which can indicate the presence of colorectal cancer or polyps. | Non-invasive, easy to perform, and can be done at home. | Less accurate than colonoscopy, may require follow-up colonoscopy if positive. |
| Stool DNA Test | A test that detects DNA changes in the stool that can indicate the presence of colorectal cancer or polyps. | Non-invasive, can detect both cancer and polyps. | Less accurate than colonoscopy, may require follow-up colonoscopy if positive. |
| Sigmoidoscopy | A procedure that uses a flexible tube with a camera to examine the lower part of the colon and rectum. | Less invasive than colonoscopy, can detect polyps and cancer in the lower colon. | Does not examine the entire colon, may require follow-up colonoscopy if abnormalities are detected. |
| Virtual Colonoscopy | A procedure that uses CT scans to create detailed images of the colon and rectum. | Non-invasive, can detect polyps and cancer. | Less accurate than traditional colonoscopy, may require follow-up colonoscopy if abnormalities are detected. |
While these alternative screening methods can be useful, colonoscopy remains the gold standard for detecting and preventing colorectal cancer due to its high accuracy and ability to remove polyps during the procedure.
Conclusion
Colonoscopy is a vital procedure that plays a crucial role in the early detection and prevention of colorectal cancer. Understanding who does colonoscopy and the importance of this procedure can help individuals make informed decisions about their health. Regular colonoscopies, performed by qualified healthcare professionals, can significantly reduce the risk of colorectal cancer and improve overall health outcomes. By following the recommended screening guidelines and discussing individual risk factors with a healthcare provider, individuals can take proactive steps to maintain their gastrointestinal health and well-being.
Related Terms:
- who gives colonoscopy
- what specialist does colonoscopy screening
- who does colonoscopy procedure
- what are colonoscopy doctors called
- provider who does colonoscopy
- who does colonoscopy test